


Dr. Kathy Monroe
Director | Professor
Dr. Mark Baker
Associate Professor
Dr. Steven Baldwin
Professor
Dr. Judson Barber
Professor
Dr. David Bernard
Professor
Dr. Sarah Bingham
Assistant Professor
Dr. Shaundra Blakemore
Assistant Professor
Dr. Jared Buchan
Instructor
Dr. Christine Campbell
Assistant Professor
Dr. Christina Cochran
Assistant Professor
Dr. Teresa Coco
Professor
Dr. Valerie Davis
Associate Professor
Dr. Shea Duerring
Assistant Professor
Dr. Pallavi Ghosh
Assistant Professor
Dr. Lynzee Head
Assistant Professor
Dr. Jaycelyn Holland
Assistant Professor
Dr. Terry Hope
Assistant Professor
Dr. Kara Huls
Assistant Professor
Dr. Ann Klasner
Professor
Dr. Edward Lose
Assistant Professor
Dr. Laurie Marzullo
Associate Professor
Dr. Jennifer McCain
Assistant Professor
Dr. Heather Mitchell
Assistant Professor
Dr. Laura Crocker Mitchell
Instructor
Dr. Michele Nichols
Professor
Dr. Melissa Peters
Associate Professor
Dr. James Sedlis
Assistant Professor
Dr. Annalise Sorrentino
Professor
Dr. Carmelle Wallace
Assistant Professor
Dr. Marjorie Lee White
Professor
Researchers in the Division of Pediatric Emergency Medicine are working on a number of multi-center studies coordinated by the National Pediatric Emergency Medicine Clinical Research Network involving infectious diseases in young infants. The division has additional important research focus areas, including:
Christine Campbell, M.D., has ongoing QI projects that include:
Christina Cochran, M.D., is part of a multi-center high powered magnet study. The first manuscript was accepted by Pediatrics, and a second manuscript is in progress.
Kara Huls, M.D., received external funding supporting her sheltered time devoted to her focus in human trafficking.
Michele Nichols, M.D., is the lead on projects, including a retrospective study on dog bites in children with Kathy Monroe, M.D., and a clonidine ingestion study with a pediatric emergency medicine fellow.
Valerie Davis, M.D., MPH, is a part of the Children’s Hospital Association Pediatric Surviving Sepsis Collaborative and the American Academy of Pediatrics (AAP) Value in Inpatient Pediatrics (VIP) QI project, Preventing High-Flow Overuse in Bronchiolitis project.
Fellow projects with faculty mentors:
Trends in Pediatric Emergency Department Acuity and Trauma during the COVID-19 Pandemic
This project was led by Shea Duerring, M.D., with participation of Isabella Masler, M.D., a pediatric resident, and Nipam Shah, Ph.D., and Kathy Monroe, M.D. This study has been submitted to Injury Epidemiology and accepted for presentation at EMS conference and Injury Free Coalition for Kids. The purpose of this study was to evaluate the effect on both volume and acuity that occurred in the pediatric population and to assist in the planning of staffing of the emergency department. The findings are seen below and have implications for staffing numbers and types of staff needed during a pandemic.
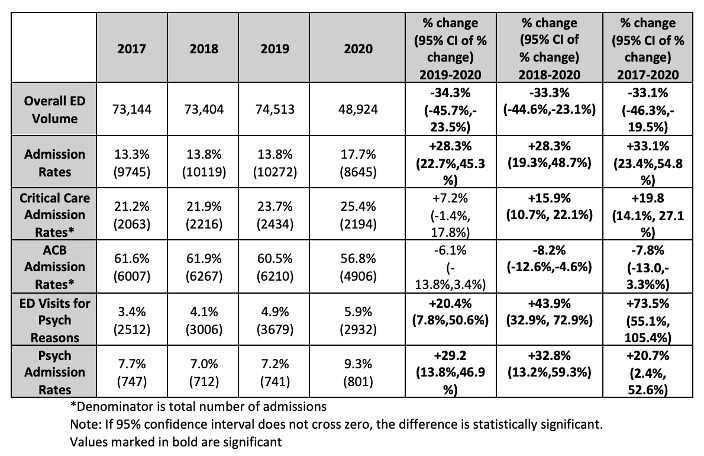
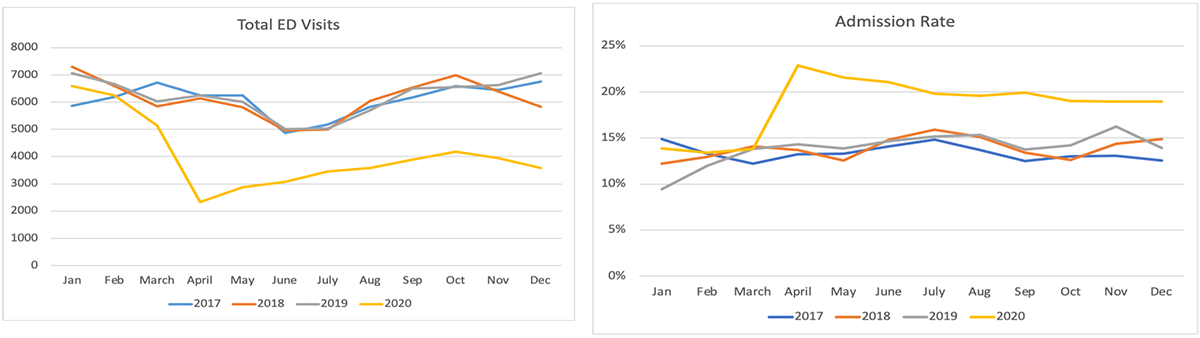
Community Partnership Approaches for Safe Sleep (CPASS)
We are one of five sites across the country to be awarded funding from the American Academy of Pediatrics. The PI for this project is Jennifer McCain, M.D., and she will be working with the Birmingham Healthy Start Plus organization and the Children’s of Alabama Foundation to provide safe sleep education to families with infants in our area. This project is much needed, as historically Alabama has one of the highest infant mortality rates in the country. This funding also provides a safe sleep environment (pack and play, sheets and safe infant sleepwear) for the families. We are particularly excited about this project, as it reaches our most vulnerable patients and provides both education and equipment to reduce one of the deadliest injuries in infants in our state.
Teen Driving Retrospective
Authors of this study published in Injury Epidemiology include Drs. Monroe and Nichols. This was an observational study of high school students ages 14 to 19 years old that compared recent self-reported risky driving behaviors to those reported in a prior study. The purpose was to assess changes in behavior and will guide interventions in the community.
Table 2. Comparison of Participant Responses from 2018 Compared to Responses in 2009
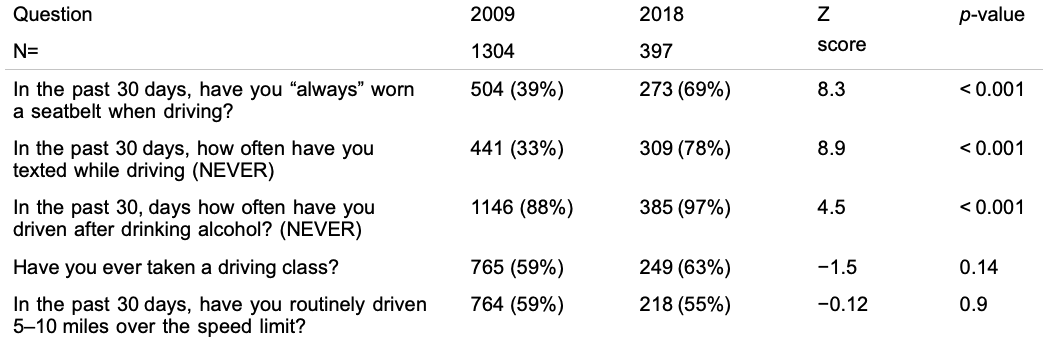
Share Our Stories: An Exploration of the Healthcare Experiences of Child Sex Trafficking Survivor Study
Carmelle Wallace, M.D., is first author on this qualitative study utilizing semi-structured interviews to explore the health care interactions of child sex trafficking survivors. Homeless youth currently aged 18–21 who were sex trafficked before age 18 were interviewed using semi-structured interview techniques.

These themes illustrate the experiences of sex trafficked youth experiencing homelessness and provide pediatric practitioners the opportunity to become more informed and equipped to recognize them.
Outpatient Pain Clinic and Intranasal Fentanyl to Improve Sickle Cell Disease Outcomes
Shaundra Blakemore, M.D., was a co-investigator on this study that has been published in Pediatric Blood Cancer. The study attempted to improve pain outcomes using an outpatient pain clinic and intranasal fentanyl in the ED pain for sickle cell order set.
TABLE 1. Comparison of outcomes for individual patient seeking care in both the pain clinic and emergency department
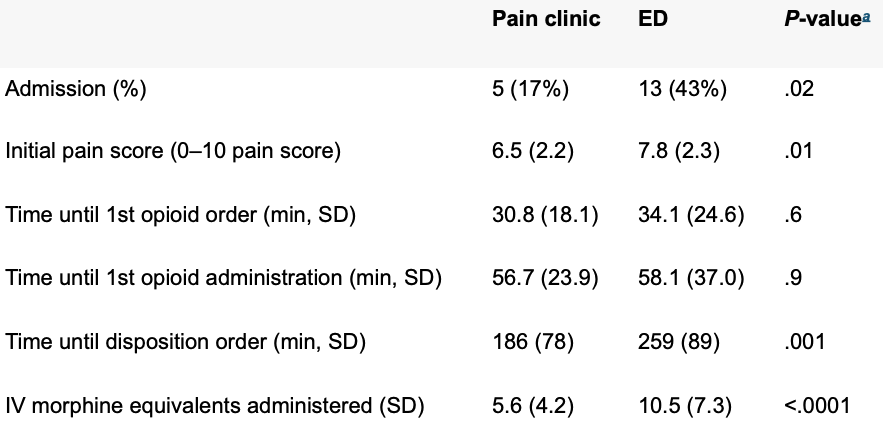
Abbreviations: ED, emergency department; SD, standard deviation.
a P-value obtained using chi-square, remaining P-values obtained using matched-pair analysis.
The use of intranasal fentanyl reduced the time to first opioid administration in the ED.
Effectiveness of a Central Line Associated Blood Stream Infection Protocol in a Pediatric Population
Dr. Monroe was a co-author on this study that was published in the American Journal of Surgery. The study focused on patients with central lines and intestinal failure (IF) who are at increased risk of bacteremia and sepsis. This was a collaborative, multidiscipline-supported protocol for the care of patients with IF presenting to the ED to enhance efficiency of antibiotic ordering/administration, as well as reduce the number of unplanned floor-ICU transfers.
Using a Resident-Led School Outreach Program to Improve Knowledge of All-Terrain Vehicle Safety
Drs. Nichols and Monroe were co-authors on this study published in Southern Med Journal. This study made use of surveillance data from the Children’s of Alabama hospital electronic medical record database. Several Alabama counties near Birmingham were identified as having an increased number of children with ATV-related injuries in 2016. The Safety Tips for ATV Riders (STARs) Program, developed in Iowa, was provided to middle school students in these counties by pediatric residents.
Acad Pediatr. 2021 Aug 10;S1876-2859(21)00424-1. Current fellowship funding limitations and their threat to the pediatric subspecialty workforce. Pnina Weiss, Angela L Myers, Kathleen A McGann, Jennifer C Kesselheim, Christine Barron, Ann Klasner, Melvin B Heyman, Doria L Weiss, Elizabeth Mauer, Katherine E Mason, Linda M Gerber, Erika L Abramson.
Academic Pediatrics. 2021 Volume 21, Issue 7, September–October, Pages 1104-1107. Social Media Changes in Pediatric Residency Programs During COVID-19 Pandemic. J Clay Pruett, Kristin Deneen, Harrison Turner, Thomas Kozar, Nikhi P Singh, Timothy W King, Michele H Nichols.
Adv Simul (Lond). 2021 Apr 29;6(1):16. Building impactful systems-focused simulations: integrating change and project management frameworks into the pre-work phase. Dubé M, Posner G, Stone K, White M, Kaba A, Bajaj K, Cheng A, Grant V, Huang S, Reid J.
American Journal of Surgery. Volume 222, Issue 4, October 2021, Pages 867-873. Effectiveness of a central line associated blood stream infection protocol in a pediatric population. M Shroyer, SA Anderson, C Hutto, K Monroe.
Cochrane Database of Systematic Reviews. Feb 2021. Belimumab for systemic lupus erythematosus. JA Singh, NP Shah, AS Mudano.
Clinical Simulation in Nursing. 2021, March. 52(C), 9-16. Interprofessional simulation for understanding poverty. Hitchcock, L. I., Timmons McKenzie, C., Shipman, S., Varley, A., Pollio, W., Peterson, D. T., King, D. M., & White, M.L.
Health Commun. 2021 Jul 12;1-9. Why We Want Our Students to Learn about Poverty and Health Care: Sharing Our Own Experiences from Poverty Simulations. Michelle Brown, Laurel Iverson Hitchcock, Dawn Taylor Peterson, Carly Timmons McKenzie, Shilpa Register, R. Lynn Holt & Marjorie Lee White.
Pediatric Emergency Care. October 2021 - Volume 37 - Issue 10 - p 498-501. Unintentional Opioid Ingestions Presenting to a Pediatric Emergency Department. Pallavi Ghosh, Christopher Pruitt, Nipam Shah, Abhay Kulkarni, Ann Slattery, Michele Nichols.
Pediatrics. 2021;147(1):e20200772. A survivor-derived approach to addressing trafficking in the pediatric ED. Carmelle Wallace, Yvette Schein, Gina Carabelli, Heta Patel, Needhi Mehta, Nadia Dowshen, Nancy Kassam-Adams, Kenneth Ginsburg, Cynthia Mollen.
Pediatrics. 2021; 148 (4). Half Century Since SIDS: A Reappraisal of Terminology. Hirsch M, B Johnston, S Kendi, LK Lee, K Monroe.
Pediatrics. Volume 147, Issue 3 March 2021. Neonatal Mastitis and Omphalitis: Presentation, Outcomes, and Concurrent Serious Bacterial Infection. Ron L Kaplan, Andrea T Cruz, Kenneth A Michelson, Constance McAneney, Mercedes M Blackstone, Christopher M Pruitt, Nipam Shah, Kathleen A Noorbakhsh, Thomas J Abramo, Richard D Marble, Leah Middelberg, Kathleen Smith, Nirupama Kannikeswaran, David Schnadower, Geetanjali Srivastava, Amy D Thompson, Roni D Lane, Julia F Freeman, Kelly R Bergmann, Oihane Morientes, James Gerard, Oluwakemi Badaki-Makun, Usha Avva, Pradip P Chaudhari, Stephen B Freedman, Margaret Samuels-Kalow, Elizabeth Haines, Jonathan Strutt, Kajal Khanna, Cheryl Vance, Lalit Bajaj.
Simul Healthc. 2021 April. An Investigation on the Perceptions of Practicing Interdisciplinary Health Professionals on Rapid Cycle Deliberate Practice Simulation. Roszczynialski KN, Register SJ, Bergman L, White ML.
Southern Medical Journal. 114.5 (2021): 266-270. Descriptive epidemiology of pediatric drowning patients presenting to a large southern US children's hospital. B Foxworthy, B Hinten, N Shah, KW Monroe, M Nichols.
Southern Medical Journal. 01 Jul 2021, 114(7):380-383. Storage of Medications: A Survey of Families in the Pediatric Emergency Department. SM Mohr, AI Atkins, AC Webb, KW Monroe, M Nichols.
Southern Medical Journal. 01 Feb 2021, 114(2):106-110. Using a Resident-Led School Outreach Program to Improve Knowledge of All-Terrain Vehicle Safety. K. Jeffries, A. Burks, M Nichols, K Monroe.
Southern Medical Journal. 2021 Jan;114(1):13-16. Examining Pediatric Residency Voting Practices. C Smola, N Shah, K Monroe.
Steve Baldwin, M.D.
Mark Baker, M.D.
Jud Barber, M.D.
Terri Coco, M.D.
Shea Duerring, M.D.
Jennifer McCain, M.D.
Kathy Monroe, M.D.
Michele Nichols, M.D.
Annalise Sorrentino, M.D.
Carmelle Wallace, M.D.
Marjorie Lee White, M.D.

Sarah Bingham, M.D.
Assistant Professor

Jaycelyn Holland, M.D.
Assistant Professor

Jennifer McCain, M.D.
Assistant Professor

Laura Crocker Mitchell, M.D.
Instructor
The UAB Pediatric Emergency Medicine Fellowship Program has been in existence for more than 30 years. We are the only Level 1 pediatric trauma center in the state and the fifth-busiest pediatric emergency department in the country. This exposes our fellows to a wide range of patient experiences and provides them with the necessary skills to become excellent emergency medicine physicians. Our fellows have an intensive didactic educational conference curriculum that includes research, quality improvement, journal club, evidence-based medicine, patient safety, radiology and interesting cases. We offer various electives and a significant amount of protected research time throughout the training program. Our research program includes online courses in epidemiology and biostatistics, lectures and mentorship with a scholarly project to be completed during fellowship.
2021–2022 Fellows
Lauren Nelson, M.D.
First-Year Fellow
Residency: St. Christopher’s Hospital for Children
Alexis Ricci, M.D.
First-Year Fellow
Residency: University of Alabama at Birmingham
Jeremy Ruhlmann, M.D.
First-Year Fellow
Combined Critical Care & Emergency Medicine
Residency: University of Alabama at Birmingham
Austin Wheeler, M.D.
First-Year Fellow
Residency: University of Alabama at Birmingham
Reid Burks, M.D.
Second-Year Fellow
Residency: University of Alabama at Birmingham
Kevin Gutermuth, M.D.
Second-Year Fellow
Residency: University of Alabama at Birmingham
Mickinzie Morgan, M.D.
Second-Year Fellow
Residency: Texas Tech Health Science Center
Eric Jorge, M.D.
Third-Year Fellow
Residency: University of Alabama at Birmingham
Emily Skoog, M.D.
Third-Year Fellow
Residency: Baylor Scott & White
Alicia Webb, M.D.
Third-Year Fellow
Residency: University of Alabama at Birmingham
Program Directors
Terri Coco, M.D.
Program Director
Christina Cochran, M.D.
Assistant Program Director
Program Coordinator
Aaliyah Williams