


Dr. Drew Davis
Director | Professor
Dr. Byron Lai
Assistant Professor
Dr. Erin Swanson-Kimani
Assistant Professor
Dr. Cynthia Wozow
Assistant Professor
The UAB Division of Pediatric Rehabilitation Medicine seeks to generate new knowledge related to disabling conditions of childhood. Through close collaboration with the UAB/Lakeshore Research Collaborative, our division is working to develop wide-reaching interventions to improve the health and wellness of children with physical impairments through sports, fitness, recreation and lifestyle interventions.
The division had a highly productive research year. Notable achievements included three publications:
The Lancet launched its third series on physical activity to review the importance of regular physical activity and sport to health and well-being, which extended the knowledge base of the previous published series in 2012 and 2016. Byron Lai, Ph.D., played a pivotal role in the physical activity series for people with disabilities. In this publication, Dr. Lai conducted systematic searches and reviews of published meta-analyses examining the benefits of physical activity on health among people living with disabilities. The results of this search are displayed in Figure 1.
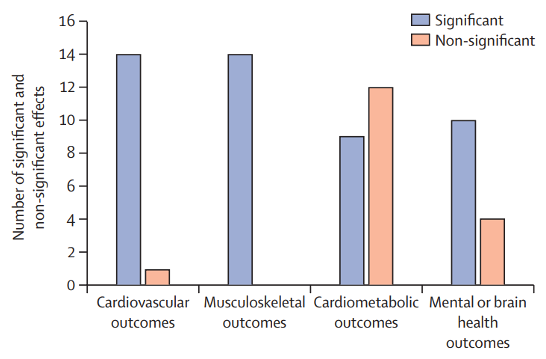
Figure 1. Number of significant and non-significant effects of physical activity interventions on cardiovascular, musculoskeletal, cardiometabolic and mental or brain health outcomes among children, adolescents and adults with disabilities. Significant average effect sizes show an advantage for physical activity versus control conditions.
In summary, high-level evidence (meta-analyses) demonstrates that participation in physical activity can elicit benefits to cardiovascular health (e.g., maximal aerobic capacity or workload and beneficial changes to skeletal muscle mitochondria) and musculoskeletal outcomes (e.g., muscular strength, power and other properties). Benefits in these health categories are similar with those observed among the general population. In contrast, beneficial changes to indicators of cardiometabolic health and mental or brain health outcomes are not well confirmed, indicating much more work is needed to develop effective interventions that target these outcomes. Examples of notable outcomes that require intervention include body composition (body weight, lean muscle mass, fat mass, etc.), blood-related cardiometabolic health indicators (e.g., blood lipids, insulin and pressure), cognitive function and emotional health. It is important to note that only 28% of the meta-analyses included children with disabilities, which indicates that far more work is needed in developing interventions that can improve health among this age group.
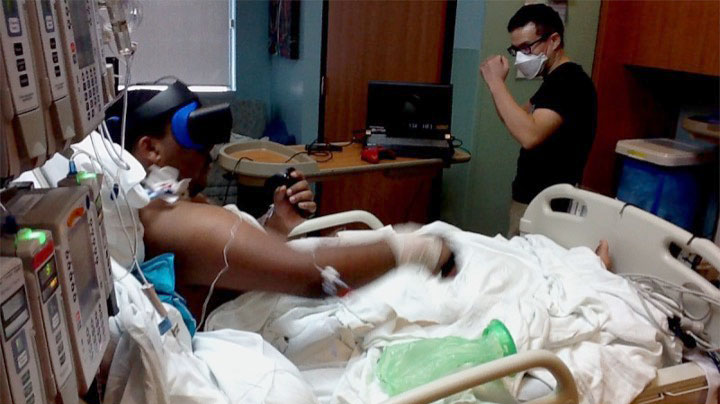
In a collaborative effort with the Early Mobility team led by Leslie Hayes, M.D., in the Division of Pediatric Critical Care, Dr. Lai created and tested the feasibility of using an innovative virtual reality system to provide two patients in the pediatric intensive care unit (PICU) with video game therapy. The results of this case study suggested that virtual reality gaming is likely a safe, enjoyable and highly desirable method of engaging certain PICU patients in early mobility therapy. Notably, the patients were cable of participating in virtual reality boxing (Figure 2) at a moderate-intensity of exercise, and this indicates that virtual reality gaming could potentially lead to health-enhancing benefits as described in the above Lancet paper. This work led to the development and submission of a Kual Pediatric Research Institute pilot grant, as well as an NIH R03 research grant.
In addition to these works, the division has just completed two research grants that were awarded within the previous year: 1) an early career research award from the American Academy of Cerebral Palsy & Developmental Medicine (AACPDM) to test an innovative scalable Movement-to-Music program among adolescents with cerebral palsy, and 2) a pilot research grant from the Center for Engagement in Disability Health and Rehabilitation Sciences (CEDHARS) examining the impact of COVID-19 on the lifestyles of adolescents with cerebral palsy who are patients at Children’s. Publications for these projects are forthcoming.
As well, Drew Davis, M.D., and Erin Swanson-Kimani, M.D., continued to collaborate with Despina Stavrinos, Ph.D. with UAB Department of Psychology to assess safety for returning to drive in adolescents who have received a mild traumatic brain injury. This work, through collaboration with the UAB Translational Research for Injury Prevention Laboratory (TRIP Lab), is funded by an NHI RO1 grant for which Dr. Stavrinos serves as principal investigator and Drs. Davis and Swanson-Kimani serve as co-investigators. This study is at the forefront of efforts nationally to learn more about the serious consequences of mild traumatic brain injury. The division also continued collaboration with leaders in the UAB Constraint Induced (CI) Therapy Research Group to develop new applications for CI therapy. This work resulted in the publication of a manuscript outlining the qualitative evaluation of Magic Camp for children with hemiplegia.
JMIR Rehabil Assist Technol. 2021 May 27;8(2):e28210. Examining the Feasibility of Early Mobilization with Virtual Reality Gaming Using Head-Mounted Display and Adaptive Software With Adolescents in the Pediatric Intensive Care Unit: Case Report. Byron Lai, Maegen Powell, Anne Grace Clement, Drew Davis, Erin Swanson-Kimani, Leslie Hayes.
J Exerc Rehabil. 2021 Feb 23;17(1):15-20. The ‘magic’ of magic camp from the perspective of children with hemiparesis. Kevin Spencer, Hon K Yuen, Gavin R Jenkins, Kimberly Kirklin, Laura K Vogtle, Drew Davis.
Lancet. 2021 Jul 21;S0140-6736(21)01164-8. Participation of people living with disabilities in physical activity: a global perspective. Kathleen A Martin Ginis, Hidde P van der Ploeg, Charlie Foster, Byron Lai, Christopher B McBride, Kwok Ng , Michael Pratt, Celina H Shirazipour, Brett Smith, Priscilla M Vásquez, Gregory W Heath.
Drew Davis, M.D. Byron Lai, Ph.D. Erin Swanson-Kimani, M.D. Cynthia Wozow, DO Byron Lai, Ph.D.Extramural Awards & Leadership Roles
New Faculty 2021

Assistant Professor